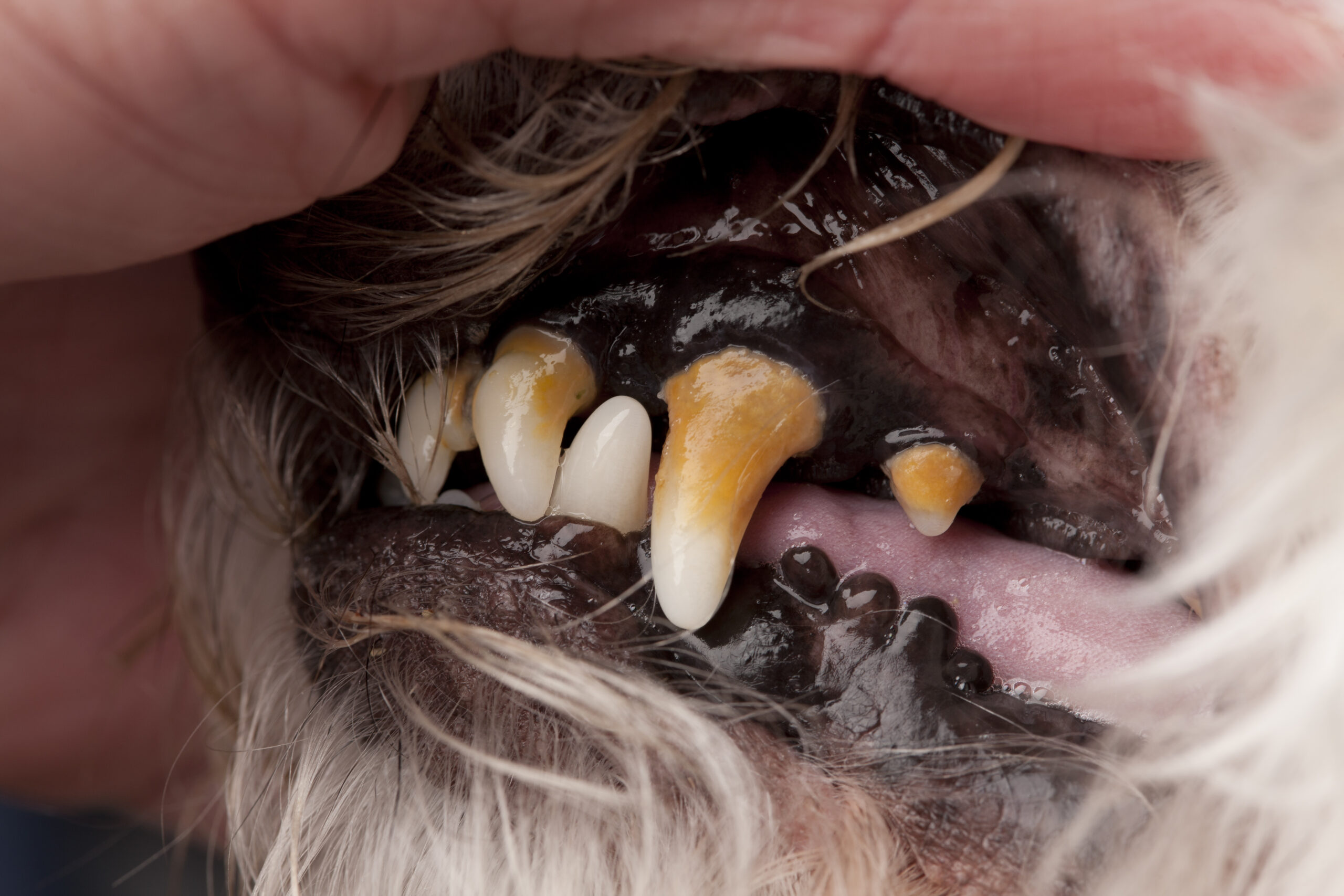
Periodontal disease is a common problem in pets, affecting most cats and dogs by age 3. While bad breath is prevalent in pets who suffer from periodontal disease, halitosis is the least of their problems. Periodontal disease can significantly impact your pet’s overall health and wellbeing.
February is National Pet Dental Health Month, and our team at Veterinary Referral Center wants to take this opportunity to provide information about periodontal disease and explain how you can protect your pet from its detrimental consequences.
What Causes Periodontal Disease in Pets?
As your pet chows down on their food, tiny particles lodge between their teeth, attracting nasty bacteria. These pathogens feed on the sugar and starches left behind and form a sticky film called plaque.
If the plaque is not removed, minerals in your pet’s saliva are deposited in the plaque biofilm, which hardens and becomes calculus (i.e., tartar). When left to multiply, the bacteria encroach under your pet’s gum line, damaging the structures that support your pet’s teeth. Periodontal disease in pets progresses in four stages:
- Gingivitis — Stage one of periodontal disease is gingivitis (i.e., an inflammation of your pet’s gingiva). The gingiva is the part of the gums around the base of your pet’s teeth. In this early phase, the disease is mild, and the supporting structures are firmly attached to your pet’s teeth. The prognosis for pets affected by gingivitis is good, as long as they receive appropriate dental care.
- Mild Periodontal Disease — As the bacteria start to break down the supporting tissues of your pet’s teeth, periodontal disease enters stage two. Less than 25% of the tooth’s supporting structures are lost at this stage. Mild bone loss may be seen on dental X-rays. The prognosis for pets affected by stage two periodontal disease is fair, as long as they receive appropriate dental care.
- Established Periodontal Disease — Stage three periodontal disease occurs when 25% to 50% of the tooth’s supporting structures are lost. Moderate bone loss may be appreciated on dental X-rays. The prognosis for pets affected by stage three periodontal disease is fair when they receive advanced dental procedures, and diligent follow-up dental care.
- Advanced Periodontal Disease — Stage four periodontal disease occurs when greater than 50% of the tooth’s supporting structures are lost. Severe bone loss may be appreciated on dental X-rays. The prognosis for pets affected by stage four periodontal disease is guarded, and any teeth damaged to this degree will need extraction.
Why Is Periodontal Disease Concerning for My Pet?
Periodontal disease can significantly impact your pet’s quality of life and overall wellbeing by causing conditions that may include:
- Halitosis — Your pet’s stinky breath is a cause for concern because the odor comes from the bacteria in your pet’s mouth. If left untreated, the condition can progress to more damaging problems.
- Oral Pain — Periodontal disease causes inflammation and pain throughout your pet’s mouth, and most pets suffer in silence until the disease is well-established. At that stage, the condition is harder to treat effectively.
- Tooth Root Abscesses — Bacteria can invade the roots of your pet’s teeth and result in painful abscesses, which can make eating and drinking difficult.
- Fractured Jaw — In cats and toy-breed dogs, severe periodontal disease can lead to a fractured jaw, since the tooth roots are so close to the jawbone edges.
- Organ Damage — Bacteria can also get into your pet’s bloodstream, and then travel throughout their body, damaging their organs, including the heart, lungs, and kidneys.
How Can I Keep My Pet’s Mouth Healthy?
While periodontal disease is extremely concerning, the condition is preventable if you take the appropriate steps to provide dental care for your pet.
Professional Veterinary Dental Cleanings
Your pet should receive regular professional dental cleanings. Most pets should have their teeth cleaned once a year starting at around age 2, but some pets, such as brachycephalic breeds, who tend to have more dental complications, may need more frequent attention.
Dental cleaning procedures are carried out under general anesthesia to ensure your pet’s safety, and to enable the veterinary professional to adequately remove the plaque and tartar from your pet’s teeth and from under their gum line. Dental X-rays are also necessary, to accurately determine your pet’s oral health status.
Toothbrushing
Daily toothbrushing is the best way to ensure your pet’s mouth stays healthy between professional cleanings.
Never use your own toothpaste on your pet, since these products can be toxic for them. Pet-specific toothpastes in a wide array of pet friendly flavors, such as poultry, beef, seafood, and peanut butter, are available, and can help your pet accept the process.
Also, ensure you use a soft-bristled toothbrush, so you don’t hurt your pet’s sensitive gums.
Dental Chews
Chewing on dental treats and toys can remove some plaque from your pet’s teeth. Choose products approved by the Veterinary Oral Health Council, to ensure they are effective.

Dr. Han Chia is VRC’s residency-trained clinician in dentistry and oral surgery. She received her veterinary degree from the University of Pennsylvania, and then completed a rotating internship at Carolina Veterinary Specialists in Charlotte, North Carolina.
Dr. Chia is passionate about all areas of veterinary dentistry and completed her residency at the Center for Veterinary Dentistry and Oral Surgery in Maryland. Her presence allows the VRC team to offer a full range of dental and oral surgery services.
If your pet has complications associated with periodontal disease, contact our VRC team, and Dr. Chia will get to the root of the problem.







 Email
Email